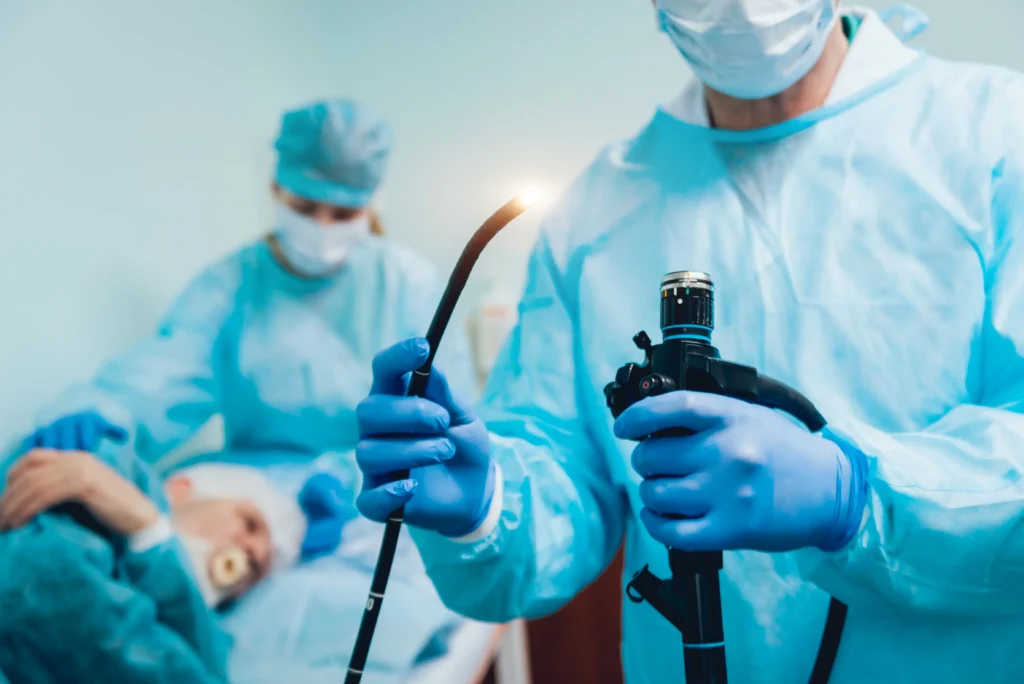
Finding answers after preventable harm.
Patients have suffered serious infections after medical procedures involving defective reusable scopes, including Endoscopic Retrograde Cholangiopancreatography (ERCP), upper endoscopy, colonoscopy, bronchoscopy, cystoscopy, and similar procedures.
These infections can lead to sepsis, repeat hospitalization, organ failure, long-term complications, and death. Food and Drug Administration (FDA) warnings, recalls, and continuing safety actions have kept contamination and reprocessing failures in focus.
If you or your family member became critically ill after one of these procedures, the key question is whether a contaminated scope or related device played a role.


How Much Is Your Case Worth?
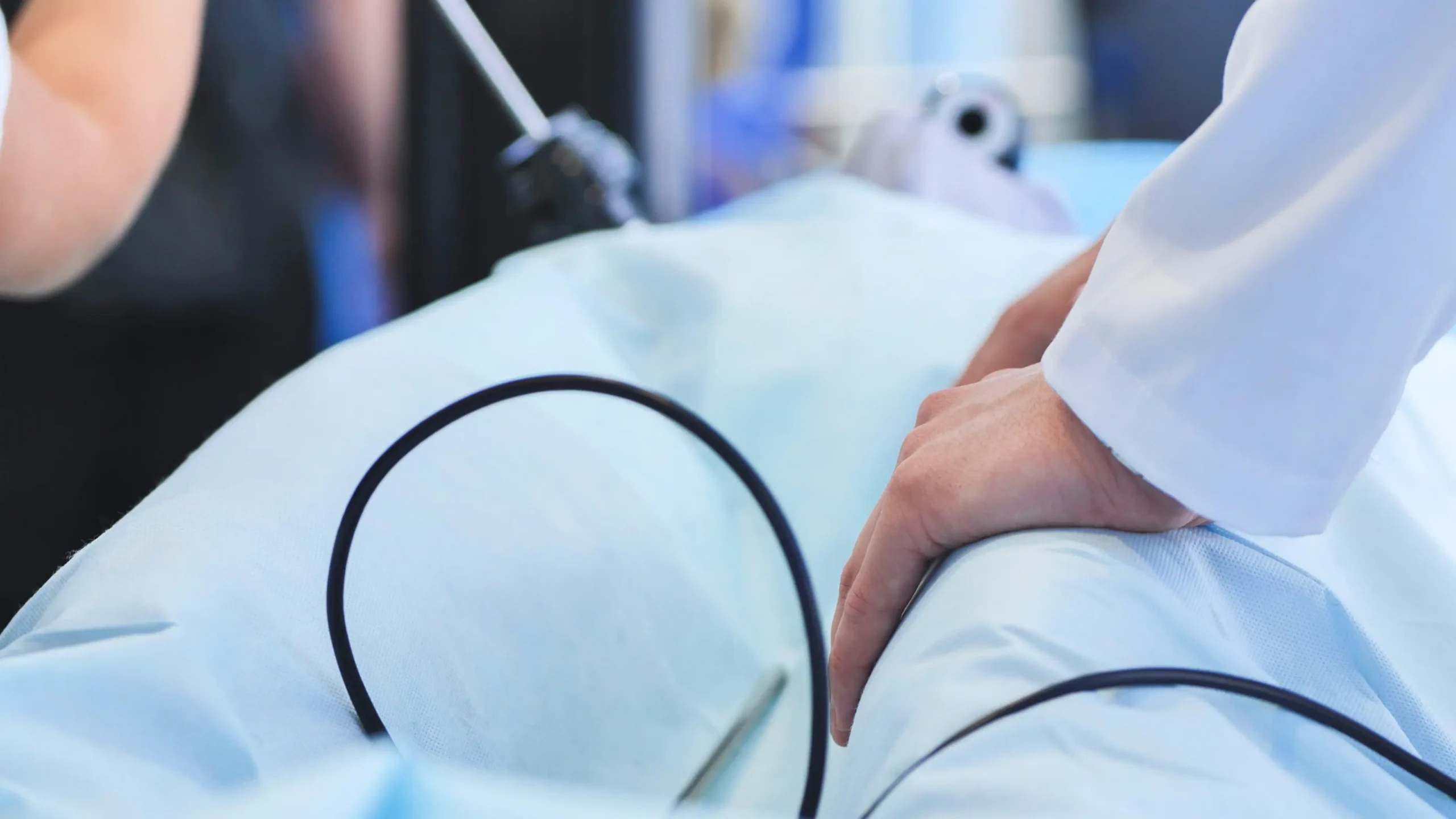
What is a scope infection case?
Scope infection cases typically involve allegations that a reusable medical scope, its components, or related reprocessing equipment exposed a patient to dangerous bacteria during a medical procedure. These claims often focus on whether a device was defectively designed, whether contamination risks were known or knowable, whether cleaning instructions were adequate, and whether safer alternatives or stronger warnings should have been used.
In product liability cases, the focus is not simply that an infection happened: the question is whether a contaminated device, a design problem, a reprocessing failure, or an inadequate warning helped cause catastrophic injury or death.
How scope infections can happen
Reusable scopes can be difficult to fully clean
Some endoscopes and duodenoscopes have intricate parts, channels, valves, and components that can make complete reprocessing difficult. If bacteria or biological material remain trapped in the device or an accessory, contamination can be passed from one patient to another.
Accessories and reprocessing equipment may matter too
The risk is not limited to the scope itself. FDA alerts and recalls have also involved accessories and reprocessing systems used with endoscopes. That matters because a contamination pathway may involve multiple products, not just the scope inserted during the procedure.
A routine procedure can become a catastrophic event
Many patients undergo endoscopy, colonoscopy, ERCP, bronchoscopy, cystoscopy, or similar procedures expecting diagnosis or treatment, not life-threatening infection. When a patient develops sepsis or another severe infection afterward, families are often left trying to determine whether the source was a contaminated medical device rather than the underlying condition alone.
Procedures that may be involved
Depending on the facts, scope infection claims may arise after:
- ERCP and duodenoscope procedures: ERCP procedures have long been central to the FDA’s duodenoscope safety actions because these devices have presented persistent reprocessing concerns. The FDA notes that duodenoscopes are used in more than 500,000 ERCP procedures each year in the United States.
- Upper endoscopy and colonoscopy: Patients may also report serious infections after upper endoscopy or colonoscopy involving reusable scopes or related accessories.
- Bronchoscopy and other scoped procedures: Bronchoscopy and other procedures using reusable scopes or accessories may raise similar contamination concerns, particularly where reprocessing problems, design issues, or hospital exposure notices are involved.
Injuries and losses linked to scope infections
A scope-related infection can escalate quickly. Reported harms in these cases may include:
- Sepsis and bloodstream infection: Sepsis is one of the most serious outcomes linked to contaminated medical devices and healthcare-associated infections.
- Drug-resistant bacterial infection: Some scope-related infection concerns have involved CRE and other antibiotic-resistant organisms that are difficult to treat. The CDC identifies CRE as a major patient-safety threat in healthcare settings.
- Organ failure and prolonged hospitalization: Severe infections may trigger Intensive Care Unit (ICU) care, repeat procedures, additional surgeries, intravenous antibiotics, and permanent health complications.
- Wrongful death: In the most serious cases, a patient does not recover. Families may be left with funeral costs, lost income, profound emotional loss, and urgent questions about what went wrong.
Recent recalls and safety actions families should know about
Scope Several recent FDA-posted actions keep this issue in focus:
- June 2025 FDA-posted duodenoscope recall: The FDA recall database shows a posted recall for the Olympus EVIS EXERA III Duodenovideoscope, Model TJF-Q190V, with the recall posted June 5, 2025.
- March 2025 FDA update on Olympus MAJ-891 accessory: The FDA stated that patient infection can occur when the MAJ-891 forceps/irrigation plug is improperly or incompletely reprocessed and that the resulting harm can include infection, urinary tract infection, sepsis, and death. The FDA update also states Olympus reported 120 injuries and 1 report of death associated with infection following procedures in which the MAJ-891 was used with a cystoscope.
- March 2026 FDA-posted endoscope reprocessor recall: The FDA posted a recall for the Olympus OER-Elite endoscope reprocessor in March 2026, identifying a compatibility problem affecting certain valves and updated reprocessing instructions.
For consumers, the important point is simple: recent recalls and safety alerts show that contamination and reprocessing concerns did not disappear. They remained active enough to generate new FDA-posted actions in 2025 and 2026.
Building a Case for Accountability
These cases are rarely straightforward. A critically ill patient may already have underlying medical conditions, multiple procedures, and a complicated hospital course. Manufacturers, hospitals, and insurers may dispute whether the infection came from the device, the procedure, the facility, or the patient’s existing health problems.
That is exactly why a careful investigation matters. The timeline, microbiology, device history, recall record, and reprocessing evidence can all affect whether a case is viable.
McEldrew Purtell’s approach includes:
- Reviewing sterilization logs, maintenance records, and infection reports
- Analyzing hospital compliance with CDC (Centers for Disease Control) and manufacturer guidelines
- Consulting infectious disease and medical device experts
- Tracing infection outbreaks to identify patterns or clusters
- Investigating prior warnings, recalls, or known device defects
We work to uncover not just what happened, but why.


Why Contact McEldrew Purtell?
When a preventable infection causes catastrophic harm or loss of life, our firm is prepared to act. We understand the complexity of these cases and the toll they take on patients and families.
Our team is committed to conducting thorough, evidence-driven investigations, holding healthcare systems and manufacturers accountable, and providing clear guidance and support throughout the legal process
If you or a loved one suffered a serious infection following a medical procedure, you deserve answers and a path forward. Contact us today for a free consultation.
Learn More
Sepsis and Serious Infections Linked to Product Defect: Contaminated Reusable Scopes
In a number of occurrences, people have gone in for routine or necessary scope procedures and come out with severe infections, repeat hospitalizations, IV antibiotics, and in some cases, death. The danger is not limited to one brand or one…
Insulin Pump / CGM Failures: Over-Delivery, Under-Delivery, and Severe Outcomes
A defective or malfunctioning insulin pump does not just create inconvenience. It can lead to under-delivery or interruption of insulin, dangerous hyperglycemia, and emergency care. FDA reports on recent corrections describe hundreds of adverse events and dozens of injuries tied…
Untraceable Firearm Product Liability: The Legal Theories Families Ask About
When a shooting involves an untraceable firearm, families often ask the same painful question: how did a weapon with no serial number and no paper trail end up in someone’s hands? These cases are sometimes described as “ghost gun” incidents,…
Surgical Mesh Complications: What “Design Defect vs. Complication” Looks Like
Surgical mesh is used in many common procedures, including hernia repair and certain pelvic surgeries. When it works, it can reinforce weakened tissue and support healing. But when patients develop serious problems afterward like chronic pain, infection, erosion, adhesion, bowel…
Spinal Cord Stimulator Paralysis Claims: What Patients Should Know After KARE 11 Investigation
A recent KARE 11 investigation reported that multiple Minnesota patients say they were left paralyzed or seriously injured after receiving spinal cord stimulator implants for pain relief at Nura Pain Clinic in Edina. According to the reporting, three patients filed…
Cleaning Agents & Product Liability
Product Liability and Cleaning Agents: What Consumers Need to Know Household cleaning agents are marketed as products that protect families from germs and harmful bacteria. When these products are contaminated, improperly manufactured, or defectively designed, they can do the opposite,…